The Campus Health Crisis No One Puts in the Brochure

Across the country, university campuses are facing a quiet but escalating crisis. It doesn't show up in rankings, it doesn't make it into guidebooks, and it rarely gets addressed in an admissions packet. But it is shaping the daily experience of millions of students in ways that affect their academic performance, their long-term health, and in the most serious cases, their lives. The crisis is access, or more precisely, the growing gap between how much care students need and how much they can actually get, for everything from a sinus infection to a skin condition to a sexual health concern to a moment when life feels like too much to carry alone.
This is not a fringe issue. It is happening everywhere, at large public universities and small private colleges, in cities and in rural towns. And it is happening right now, at the exact moment when students need support most.
The Reality of Student Health Today
College is often framed as one of the most exciting times in a person's life, and for many students it is. But it is also one of the most medically vulnerable. Students are leaving home for the first time, navigating independence, managing social and academic pressures, and constructing their identities often simultaneously. That convergence of transition stressors creates a surge in health needs across every dimension, physical, emotional, and everything in between, frequently at the same time.
The physical health reality alone is significant. According to the American College Health Association, respiratory illness, infections, skin conditions, and injuries are among the most common reasons students seek care, and yet a large share never do. Students arrive on campus managing chronic conditions that were handled at home, by a parent who scheduled the appointments, filled the prescriptions, and knew the family doctor by name. That infrastructure disappears the moment they move into a dorm. Add congregate living, irregular sleep, inconsistent nutrition, and the physical stress of academic pressure, and you have a population with substantial ongoing medical needs and shrinking access to care.
That complexity is compounding. Today's students arrive managing a wider range of overlapping conditions than any previous generation, from chronic physical conditions, like asthma and hypertension, and shifting hormonal health to ADHD, autism spectrum disorders, and evolving questions about sexual and reproductive health, often for the first time, without a parent or family doctor to help navigate any of it.
What makes this moment distinct is not just that students have more health needs, it is how they expect those needs to be met. Today's college students, part of Gen Z, have grown up with on-demand everything. They order food, stream content, and connect with friends instantly, on their terms, without friction. They bring those same expectations to healthcare—and when the system requires them to call ahead, schedule a week out, cross campus, and sit in a waiting room, many simply opt out. Not because they do not value their health, but because the experience feels incompatible with how they actually live. The students most likely to delay care are not indifferent to their well-being—they are unwilling to navigate a system that was not designed for them. That gap between expectation and experience is where early health problems quietly become serious ones.
The mental health picture compounds that reality in ways that cannot be ignored. According to the 2024–2025 Healthy Minds Study, over a third of college students experience moderate-to-severe depressive symptoms, and fewer than four in ten report actively flourishing. These numbers matter because mental health is inseparable from physical health. A student with untreated anxiety is more likely to get sick, including physical symptoms, less likely to seek care, and more likely to fall behind. The two are not separate systems, and a campus health model that treats them that way will always fall short.¹
Why the Existing Model Is Breaking Down
Most universities already have health centers or infirmaries. So why are so many students still struggling to get care?
The answer is structural. Campus health models were largely designed for a different era, built around centralized facilities, business-hour availability, and a presumption that students could and would schedule appointments, travel to a clinic, and navigate a system that sometimes feels more like a bureaucratic hurdle than a front door to care.
That model is straining under the weight of current demand. Campus counseling centers are significantly understaffed relative to the populations they serve. The International Association of Counseling Services recommends a ratio of one full-time professional staff member for every 1,000 to 1,500 students. At many major universities, that ratio runs closer to one professional per 3,000 to 4,000 students, meaning the gap between what is recommended and what exists is often measured in thousands of students per clinician.² The same capacity problem exists on the physical health side, where health center wait times, limited hours, and single-location access leave students choosing between skipping class to see a provider or skipping care altogether.
What makes this structural problem so striking is that it persists even at institutions actively trying to solve it. Some of the most well-resourced universities in the country have invested heavily in modernizing—expanding clinic locations, adding telehealth portals, building scheduling apps, launching wellness platforms, and redesigning intake models around access for both physical and mental health care. These are not small gestures.
And yet the structural ceiling remains. Wait times for both physical and mental health services stretch two to three weeks at many institutions, and beyond a month at some. Health centers operate during business hours while student health needs do not. Session caps, referral requirements, and single-location facilities mean that even students who seek care often can't complete it. When students work up the courage to ask for help and are told the next available slot is weeks away, many simply don't come back. By the time a slot opens, the moment that drove them to seek help may have passed, unresolved.
The consequences are sharpest at rural and regional campuses, where the health center is often the only provider within reach, for physical or mental health care alike. When a student at a rural four-year university hits a waitlist or a capacity limit, there is no urgent care clinic nearby, no community provider down the street, and no off-campus safety net to absorb the overflow. Research confirms that rural campuses often see the highest utilization rates of any institution type—because students have no alternative. The demand is greatest exactly where the backup resources are thinnest.
The digital investments universities have made tell the same story. Telehealth portals, scheduling apps, and wellness platforms have proliferated across campuses—and yet adoption remains low. The reason is friction. Logging into a portal, selecting a provider, scheduling a future appointment, finding a private space to take a video call—each step is a decision point where students opt out. Gen Z navigates on-demand digital services fluently, but they abandon experiences that require effort, navigation, or waiting. A scheduling app is not the same as immediate access.
Transportation compounds the problem. Roughly 40 to 50 percent of students, particularly freshmen, do not have access to a vehicle. Off-campus care is not a realistic option for a student between classes on a Tuesday afternoon. Even on-campus care is often located in a single facility that requires intention, transit time, and scheduling to reach.
Then there is the issue that does not get discussed enough: privacy. Dorm rooms are shared. Libraries are public. Campuses are, by design, social environments. There are very few places where a student can speak openly or seek care without worrying about being seen. And that barrier is not limited to mental health. A student managing a sexual health concern, a reproductive health question, a chronic condition they have not told their parents about, or a struggle with substance use faces the same problem. The absence of a private, judgment-free space to seek care is one of the most under appreciated reasons students delay, avoid, or abandon the care they need.
Stigma is not just a feeling. It is a structural barrier that prevents care-seeking across every health category, and any model that does not account for it will always leave students behind.
The common thread is not negligence. It is architecture. Every model, however thoughtfully designed, still requires students to schedule, come, and wait for care. And that requirement, invisible as it seems, is where students are lost.
Why College Campuses Are Ground Zero
Here is what makes this moment so consequential. The college years are not just academically formative. They are medically formative. Chronic conditions including hypertension, diabetes, and respiratory disease often begin their silent progression during this window, long before a diagnosis is made. Unhealthy patterns established in college, around sleep, nutrition, physical activity, and care-seeking behavior, have a way of becoming permanent. Students who do not learn to access care, or who learn that care is inaccessible, carry that lesson with them for decades.
At the same time, 75% of all lifetime mental health disorders present by age 24, making the college campus ground zero for early identification and intervention on that front as well. The students sitting in dining halls and dorm rooms right now are at the developmental window where early support, across both physical and mental health, can meaningfully alter the trajectory of a life. Miss that window, and the opportunity to intervene may not come again.
Poor service utilization during this period is alarming across both dimensions. Effective early management is key not only to preventing the progression of physical and mental health conditions, but also to reducing the long-term consequences so often associated with undetected, untreated disease.³
The cost of inaction is not abstract. It shows up in dropout rates, in academic underperformance, in chronic conditions that begin in college and persist for decades. Research shows that 68% of students indicated their health difficulties had impacted their academic performance in the past month.⁴ The American College Health Association consistently finds that physical health concerns, including respiratory illness, sleep disruption, and chronic conditions, rank among the leading reasons students miss class, fall behind, or disengage entirely. These are not just wellness statistics. They are retention and outcomes issues that universities are increasingly being asked to address with constrained budgets and legacy infrastructure.
What a New Model Looks Like

What if care did not require an appointment? What if it did not require crossing campus, arranging transportation, or walking through a visible clinic door? What if care was private and stigma free? What if the system met students exactly where they already are?
That is precisely what OnMed's CareStation™ makes possible.
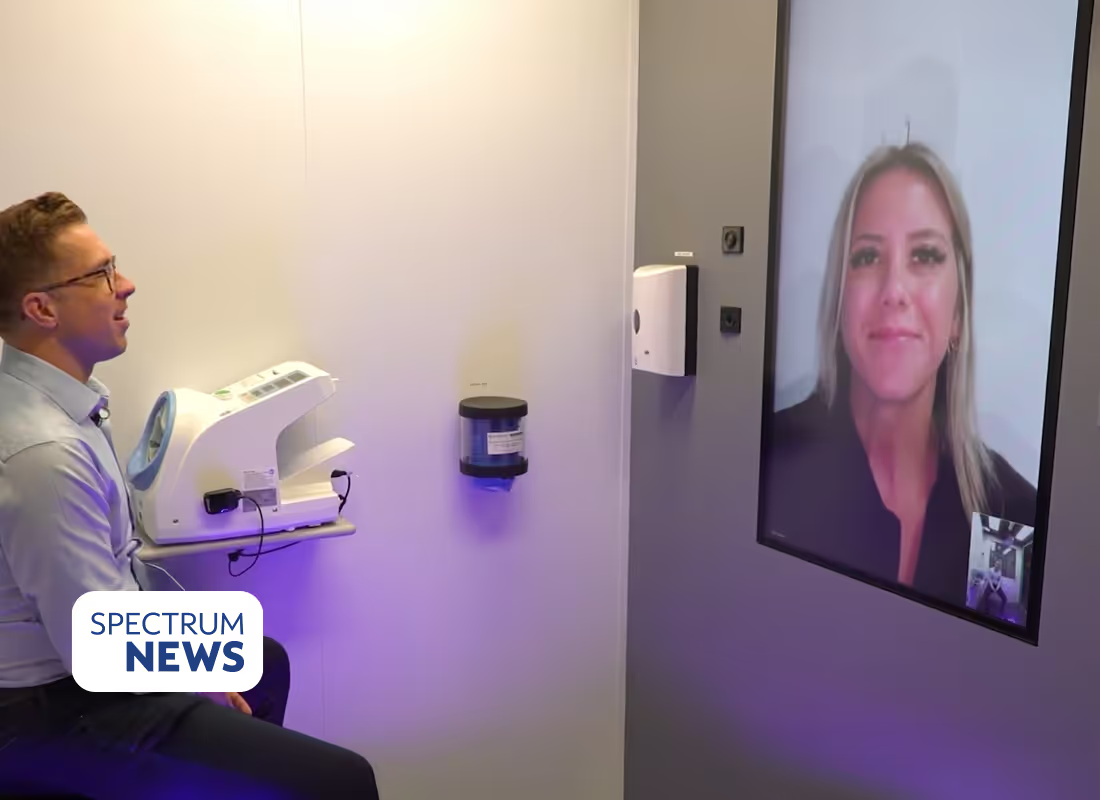
The CareStation is a patented, 8x10 foot healthcare environment that can be deployed directly into student unions, dining halls, residential hubs, and other high-traffic campus spaces. It is not a passive telehealth kiosk. It is a fully integrated "Clinic-in-a-Box" with provider-led care and the tools to diagnose, bringing clinical-grade capability to the places students already spend their time.
Inside the CareStation, students have access to advanced diagnostic tools including high-definition cameras, a digital stethoscope, blood pressure monitoring, pulse oximetry, thermal imaging, scale, and otoscope. These are not screening tools. They are the instruments of comprehensive clinical evaluation, enabling accurate assessment and treatment without a referral or a follow-up appointment somewhere else. In fact, more than 85% of OnMed users are fully diagnosed without specialist referral.

The care is tech-enabled and AI-powered, with intelligent clinical workflows that guide intake, identify risk signals, and support decision-making. But it is always human-delivered at the last mile. Every student who uses the CareStation is connected to a licensed clinician who provides judgment, empathy, and trust. The AI makes care faster and more accurate. The human makes it real.
Conditions treatable through the CareStation span a broad and meaningful range of the health concerns students actually face: cold, flu, respiratory illness, fever, sore throat, allergies, asthma, skin conditions, minor injuries, common infections, sexual health concerns, chronic condition monitoring, and preventative screenings. These are the everyday, urgent, and often private health needs that students currently navigate without a convenient or confidential place to go. The CareStation gives them one.
Today, the CareStation also includes mental health screenings for anxiety and depression, and clinicians trained in suicide ideation recognition, so that a student who comes in for a physical concern and mentions they have been struggling emotionally is never sent away without support. That screening capability is not a footnote. On a campus where stigma prevents most students from ever walking into a counseling center, having a trusted, private, judgment-free space that can identify mental health needs in the same visit as a sinus infection is genuinely significant. Beginning in Q4 2026, the CareStation will expand further, integrating licensed mental health professionals who can deliver full therapeutic sessions and comprehensive behavioral health care, not just screenings, but ongoing treatment for anxiety, depression, acute emotional distress, burnout, and sleep challenges. The physical health platform delivers real, comprehensive care right now. What is coming in Q4 2026 will only deepen that impact.
Critically, students can access all of this in a completely private, stigma-free setting. No one knows whether the student who just stepped inside is managing a chronic condition, asking a question they are too embarrassed to ask anywhere else, or simply dealing with a sinus infection. That anonymity is not incidental. It is architecturally intentional, and it removes one of the most persistent barriers to care-seeking that students face.
Already Working. Already Here.
OnMed is already proving the model works. The CareStation is currently deployed on university campuses in three states, serving students, faculty, and staff with the kind of immediate, private, whole-person care this blog describes. The results speak for themselves: 86% of users report the CareStation as their primary place for care, with an average patient satisfaction score of 4.95 out of 5. 92% of visits result in full diagnosis and treatment without specialist referral, and 40% of users are repeat patients, a signal that students are not just using the CareStation once out of curiosity, they are making it a habit. In a population where getting a student to seek care at all is half the battle, that kind of repeat utilization is meaningful. Universities that have deployed the CareStation have seen measurable reductions in health center congestion, and students who might never have sought care at all are now accessing it regularly, right where they live and study.
At South Carolina State University, the experience speaks for itself. Dr. Audrey McCrary-Quarles, Co-Director of the Health Education Research and Training Center, has watched the dynamic firsthand. "Students will actually be students, and it's hard to get them to focus on health at an early age," she said. "But they will come to the OnMed CareStation if they have something going on at that moment. And once they do, they don't only come for their health, they become advocates on campus with their peers. They go home and tell their family members. When other students are sick, they say, did you go to the OnMed CareStation? It's no cost. It's accessible. You don't have to worry about anyone knowing your information. It's confidential."
The Economics Make Sense
Universities are under increasing pressure to do more for student well-being while managing constrained budgets. The CareStation model changes that equation.
At scale, the cost of deploying a CareStation can be as low as one to two dollars per student per month. To put that in context: average published tuition and fees for private nonprofit four-year institutions reached $45,000 for the 2025–2026 academic year. At that rate, comprehensive on-campus care infrastructure represents less than one-tenth of one percent of annual tuition. Students and families will not feel that cost. And universities get a model that is more cost-effective than expanding facilities, less resource-intensive than hiring additional full-time staff, and capable of meaningfully reducing strain on the existing health center infrastructure.
The CareStation is not a replacement for campus health services. It is a force multiplier, extending reach, expanding access, and absorbing demand for the kinds of episodic, immediate care that currently floods health centers and infirmaries during peak periods like midterms and finals week.
The value of a CareStation on campus does not stop at the student population. Faculty and staff are an often-overlooked beneficiary of on-campus care infrastructure, and universities are, at their core, large employers. According to the Integrated Benefits Institute, illness-related lost productivity costs U.S. employers $575 billion annually, nearly 1.5 billion days of lost work driven by absence, disability, and chronic health conditions that go unmanaged until they become crises. On a university campus, that cost is not just financial. When faculty miss class, when advisors are out, when the counselor a student finally worked up the courage to see is unavailable, the student experience suffers in ways that are hard to measure but easy to feel. When faculty and staff have access to convenient, on-site care, they are far more likely to address health concerns early, before those concerns become absences. A CareStation deployed in a shared campus space serves the whole community, extending the return on investment well beyond the student body and positioning the university as an employer that genuinely takes the health of its people seriously.
A Competitive and Strategic Differentiator
There is a commercial dimension to this conversation that university leaders should not overlook. Healthcare access is increasingly influencing where students choose to attend college. Students and parents are asking directly: will I be supported? What happens if something goes wrong? Can I get care without waiting three weeks?
A university that deploys the CareStation can answer those questions with confidence. Students will have immediate, private, on-demand access to comprehensive physical health care, right where they live and study, any time they need it, with mental health screening and support available in the same private space today, and fully integrated behavioral health care arriving in Q4 2026. That is a meaningful and differentiating answer in an enrollment landscape where well-being is becoming a competitive dimension. It positions the institution as innovative, student-centered, and genuinely committed to whole-person health, not just academic outcomes. It gives parents peace of mind, and it gives students a reason to choose, stay, and succeed.
Beyond the Campus Borders
For institutions where community engagement is embedded in the mission, the CareStation extends that commitment beyond enrolled students. With the right deployment model, CareStations can support broader community health initiatives, provide care infrastructure during public health events, and serve as a meaningful resource in times of crisis.
That last point is worth sitting with. The next major public health event is not a question of if. It is a question of when. Universities that have already built out healthcare access infrastructure will be in a fundamentally different position than those that did not. The investment in a CareStation today is also an investment in institutional resilience tomorrow.
The Future of Campus Health
The traditional model of centralized, appointment-based, single-facility health services was never designed for the scale, the complexity, or the urgency of student health needs in 2026. Students need immediate access, privacy, and integrated physical and mental health care. They need support that fits the way they actually live, not the way health systems were historically designed.
Earlier intervention means better outcomes. It means less strain on existing systems. It means students who stay enrolled, perform better, and graduate healthier than they arrived. And it means universities that can honestly say they are doing something real about student well-being, not just talking about it.
The CareStation meets students where they are. That is where care has always needed to be.
Learn more about how OnMed provides comprehensive, immediate healthcare directly in schools and universities here.
Sources
- Healthy Minds Network. 2024–2025 Healthy Minds Study. University of Michigan School of Public Health, 2025.
- International Association of Counseling Services. Accreditation Standards. As cited in The OU Daily, December 2024.
- McGorry, P.D. et al. "Early intervention in youth mental health: progress and future directions." PMC, 2023.
- Center for Collegiate Mental Health. 2024 Annual Report. Penn State University, 2024.
- American College Health Association. National College Health Assessment. 2024.
- Inside Higher Ed / Healthy Minds Study. "College Student Mental Health Remains a Wicked Problem." October 2025.
- College Board. Trends in College Pricing 2025–2026. CollegeBoard Research, 2025.
- The OU Daily. "Goddard Health Center's limited staff, tight budgets mean long wait times." December 2024.
- Integrated Benefits Institute. "Poor Health Costs US Employers $575 Billion and 1.5 Billion Days of Lost Productivity." December 2020.
About OnMed
OnMed is transforming how the world accesses healthcare. With its patented OnMed CareStation™, an 8×10 foot “Clinic-in-a-Box”, OnMed delivers comprehensive, immediate care wherever people live, work, and learn. The OnMed CareStation™ is a tech-enabled, AI-powered, and human-delivered platform that blends the comprehensiveness of traditional in-person care with the rapid scalability of telemedicine. Each CareStation serves as a local access point within a scalable, connected grid that delivers everyday healthcare at scale.
Powered by public-private partnerships across insurers, healthcare providers, governments, employers, and educational institutions, OnMed is redefining healthcare access, closing critical gaps, restoring trust, and strengthening the health and economic resilience of communities everywhere. Learn more at www.onmed.com.
.avif)












.avif)


.avif)




















































.avif)















