How Health Systems Are Reducing ED Strain, Cutting Leakage, and Expanding Access Without Building

Two Directions. Total Control of the Patient Journey.
How the OnMed CareStation™ simultaneously expands your catchment zone, eliminates uncompensated ED waste, closes referral leakage, and turns clinician burnout into a retention opportunity—through a single, AI-powered platform.
Revenue leaks out through patient leakage, LWBS, and referral loss. Costs climb through uncompensated ED care, readmissions, and clinician burnout. Most access strategies address one side of that equation. The OnMed CareStation™ addresses both—simultaneously.
The Healthcare Access Problem Has Two Edges. Most Strategies Only Address One.
Health systems spend enormous capital and strategic energy trying to solve the healthcare access problem. New urgent care locations. Telehealth platforms. ED capacity expansions. Physician recruitment in underserved ZIP codes. These are not wrong investments, but they share a fundamental limitation: they're unidirectional. They either improve what happens inside your walls, or they attempt to reach out into the community. Rarely both, and almost never simultaneously.
The result is a gap. Patients leak out of your network to competitors. Non-emergent cases flood your ED and consume resources without generating equivalent revenue. Readmission rates climb because post-discharge follow-up is too friction laden. And clinical staff burn out managing a volume and acuity mismatch that was never supposed to be their burden.
The OnMed CareStation™ was engineered to close all these gaps at once—through what we call the Outside-In / Inside-Out dual strategy. Two simultaneous, self-reinforcing motions that, together, give your health system something most have never had: end-to-end control of the patient journey.
Outside-In: Own the Catchment Zone
• Place branded CareStations at employers, senior facilities, schools, and retail sites
• Extend your catchment zone beyond physical geography
• Intercept patients before they find a competitor
• 100% of referrals route within your network
• Reduce readmissions through post-discharge community access
• Build loyalty through consistent, branded touchpoints
Inside-Out: Optimize the Foundation
• Deploy CareStations in ED waiting areas and hospital campuses
• Triage and route L4/L5 non-emergent patients before they consume ED resources
• Reduce LWBS and keep patients engaged while alleviating bottlenecks
• Maintain EMTALA compliance with a documented, auditable workflow
• Free clinical staff to focus on true emergencies
• Offer CareStation access as a 24/7 benefit for your own provider staff
Executed together, these two motions close the loop. You're not just improving what happens at the front door, you're ensuring that patients who encounter your brand anywhere in the community find their way into your system, get excellent care, and stay there for every downstream encounter their condition requires.
Outside-In Strategy: Community Access, Expand Without Building

Your Catchment Zone Is Whatever You Make It.
Health system growth used to mean capital investment: land, construction, equipment, staffing, regulatory approvals. A new clinic adds access, but it costs $2–5M before the first patient walks in, and it serves only the geography immediately around it. The CareStation changes the fundamental economics of access expansion.
A CareStation can be deployed at an employer site, a senior living facility, a school campus, or a retail location in weeks, not years—and at a fraction of the cost. Every unit is branded with your health system's identity. Every patient who uses it is your patient. Every referral that follows goes into your network.
The CareStation delivers results: 86% of patients are treated without requiring ED escalation, 100% of referrals are directed within your health system network, and more than 50% of users present with an undetected or unmanaged chronic condition.
Prevent Leakage. Capture Patients for Life.
Patient leakage is one of the most significant and least visible revenue drains in health system finance. A patient who sees a cardiologist outside your network doesn't just cost you one specialist visit, they cost you every downstream encounter that cardiology generates: imaging, labs, follow-up, interventional procedures, hospitalization. The lifetime value of a captured patient is enormous. The lifetime cost of a leaked one compounds in your competitor's favor.
Every CareStation in the community refers 100% of patients within your network. The patient who steps into your branded CareStation for a blood pressure check walks out with a follow-up appointment scheduled, with a cardiologist, a PCP, or a specialist, all within your system. The referral loop closes before they ever have a chance to look elsewhere.
Reduce Readmissions Through Post-Discharge Access
CareStations at community sites also solve one of the most persistent drivers of readmission: the gap between discharge and follow-up. When a patient is discharged with instructions to follow up in 7–10 days, the reality of navigating a scheduling system, arranging transportation, and taking time off work creates friction that turns "I'll follow up" into "I'll wait until it gets worse." A CareStation in their workplace or community removes every one of those barriers and keeps the post-acute relationship inside your system.
The Employer Deployment Play
For health systems, employer partnerships represent a contracted deployment with a guaranteed patient population—a community access point that generates in-network referrals from day one. Employers are actively searching for ways to reduce healthcare costs and improve workforce productivity. A CareStation on-site or at a nearby location serves both goals—reducing absenteeism, eliminating the need for off-site urgent care visits, and delivering care that keeps employees in-network. For the employer, it's a measurable benefit. For the employee, it's the most convenient care they've ever had access to.
Population Health Starts in the Community
Approximately one-in-three patients who use the CareStation present with a chronic condition that is either undetected or unmanaged. That's not a coincidence. It reflects the reality that millions of Americans avoid or delay care until symptoms force them to act. By placing the point of care at the employer, the senior facility, or the retail site, the CareStation intercepts these patients at the earliest possible moment in their clinical trajectory.
Early detection means lower-acuity treatment. Lower-acuity treatment means better outcomes, lower cost-of-care, and a patient whose chronic condition is now managed, and monitored, within your system. The AI platform powering each CareStation learns population patterns over time, enabling your clinical leadership to see trends, flag at-risk cohorts, and design interventions before conditions escalate into high-cost encounters.
Inside-Out Strategy: ED Optimization

The Outside-In strategy captures patients in the community. But what about the millions of newly uninsured patients already heading toward your ED?
Millions Are Losing Coverage. Here's What It Means for Your Health System.
The Medicaid landscape has undergone a seismic shift—and the reverberations are heading directly toward your emergency department. Between April 2023 and mid-2025, more than 25 million people were disenrolled from Medicaid during the post-pandemic coverage unwinding.[1] Nearly 70% of those lost coverage for procedural reasons—not because they were ineligible, but because they couldn't navigate the renewal paperwork.[2] And the disruption is far from over.
Ongoing changes to Medicaid eligibility rules, including new work and documentation requirements taking effect in 2027, are projected to result in millions more losing coverage in the years ahead. Independent analysis estimates these coverage shifts could generate approximately 94,800 preventable hospitalizations and leave 1.6 million people delaying care due to cost, every year.[3,4] Regardless of where one stands on the policy merits, the operational consequence for health systems is the same: more uninsured patients seeking care, with fewer coverage pathways to pay for it.
Research consistently shows that loss of Medicaid coverage, even temporarily, leads to more hospitalizations and ER visits.[5] When coverage erodes at scale, a significant portion of those affected don't stop needing care. They show up at the nearest emergency department, because EMTALA guarantees they'll be seen. The uncompensated care burden your ED already absorbs is set to grow, unless you intercept these patients before they get there.
The Patient the ED Was Never Designed to Lose: The Insured LWBS
Here is the dynamic that rarely appears in the financial models but is playing out in waiting rooms across the country every day: the influx of uninsured, non-emergent patients consuming ED capacity doesn't just cost money on the uncompensated care line. It displaces paying patients who leave.
Patients who leave the emergency department without being seen—known as LWBS—represent a direct and measurable revenue loss. Research from the Western Journal of Emergency Medicine places the average revenue loss per LWBS patient at approximately $687 in direct ED fees alone.[6] When downstream inpatient admissions are factored in, each LWBS represents a potential loss of $10,000 or more to the health system.[7] For a hospital running a 3–4% LWBS rate on 70,000 annual visits, that's a conservative seven-figure revenue gap, every year, from patients who wanted to pay you and left because they couldn't wait.
Research shows that nationally, 3.2% of ED patients leave before treatment is complete,[8] each representing a potential loss of ~$10K to the health system when downstream admissions are factored in—and 78% of those leaving are insured adults.
Who are the patients leaving? Research paints a specific and commercially significant portrait. A large multicenter study found that LWBS patients who did not seek follow-up care were disproportionately younger, female, and non-White, presenting with lower-acuity complaints that were entirely treatable.[9] A separate study found that the majority of non-urgent ED visits—nearly 78%—were actually made by insured adults, not the uninsured.[10]
These are insured patients with primary care providers who came to you with an acute need and no convenient alternative—and because your waiting room was overwhelmed by EMTALA-mandated non-emergent volume, they left and took their lifetime of care to a competitor.
The insured patient who leaves your waiting room doesn't just cost you that visit. She costs you every encounter she would have generated over a lifetime of care—and she takes that lifetime to whoever saw her next.
Your ED Was Never Designed to Be Primary Care.
ED optimization starts with understanding how it got there. But in the absence of accessible alternatives, especially for the uninsured, it became exactly that. EMTALA requires hospitals to evaluate and stabilize every patient who presents at the ED, regardless of ability to pay or acuity level. That's not a flaw in the law; it's a vital patient protection. But it creates a structural cost burden that falls entirely on the health system. With coverage shifts already underway and more projected in the years ahead, the uncompensated care equation is only moving in one direction.
Studies consistently show up to 40% of ED visits are classified as non-emergent or low-acuity. Uninsured patients who lose Medicaid coverage don't stop needing healthcare. Research shows that gaps in Medicaid coverage reliably drive more hospitalizations and emergency visits.[5] These patients are not bad actors, they're following the only path available to them. The problem is systemic. So is the solution.
U.S. health systems absorb $45B in annual uncompensated ED care, while $168B is wasted each year on non-emergent and avoidable ED utilization—and 63% of ED clinicians report burnout, with volume mismatch cited as a primary driver.
The EMTALA-Compliant CareStation Workflow
Health system leaders evaluating any ED triage solution need confidence that EMTALA compliance is airtight. The CareStation Inside-Out workflow is built from the ground up around EMTALA compliance. There is no shortcut, no grey area, and no compliance exposure. Here's how it works:
- Patient Presents- Patient arrives at ED and is registered per standard protocol
- Medical Screening Exam- Qualified medical professional conducts the required MSE
- No EMC Documented- No emergency medical condition identified and documented in the record
- CareStation Transition- Patient is offered and consents to transition to the CareStation
- Treated & Referred- Patient receives full diagnostic workup, Rx if needed, and follow-up referral within network
Critically: the ED still bills for the visit. The Medical Screening Exam is a billable service. Revenue is not lost, waste is eliminated. The patient gets faster, more dignified care. The ED regains capacity for the patients who genuinely need it.
Full Diagnostic Capability. Not a Kiosk.
The CareStation is not a check-in terminal or a symptom screener. It is a fully equipped clinical environment, AI-powered and clinician-supervised, capable of delivering comprehensive primary and urgent care for a wide range of conditions.
- Vitals & Monitoring- Blood pressure, pulse ox, heart rate, temperature, BMI, respiratory rate
- Diagnostic Scopes- Otoscope, ophthalmoscope, stethoscope — all transmitted digitally
- Rapid Lab Testing- Flu A/B, Strep, COVID, UTI, and additional point-of-care panels
- Prescription Authority- AI-assisted clinical decision support with supervising physician authorization
- Specialist Referral- Warm handoff referrals directly into your network scheduling system
- Chronic Condition Detection- Hypertension, diabetes risk, respiratory conditions, and more
The CareStation as a Staff Benefit
The CareStation isn't only for patients. Your own clinical and administrative staff can access it as an on-site healthcare benefit, receiving fast, comprehensive care for minor illnesses without leaving campus, disrupting their schedule, or waiting in the same ED they work in. In an environment where 63% of ED clinicians report burnout, offering a dedicated, private, zero-wait care option for your own team sends a signal that matters: your institution invests in the people who power it.
The ROI Is Structural, Not Incidental.
The CareStation is not a cost center dressed up as innovation. Each deployment creates measurable, compounding returns across your financial, operational, and workforce metrics. Here is the consolidated case:
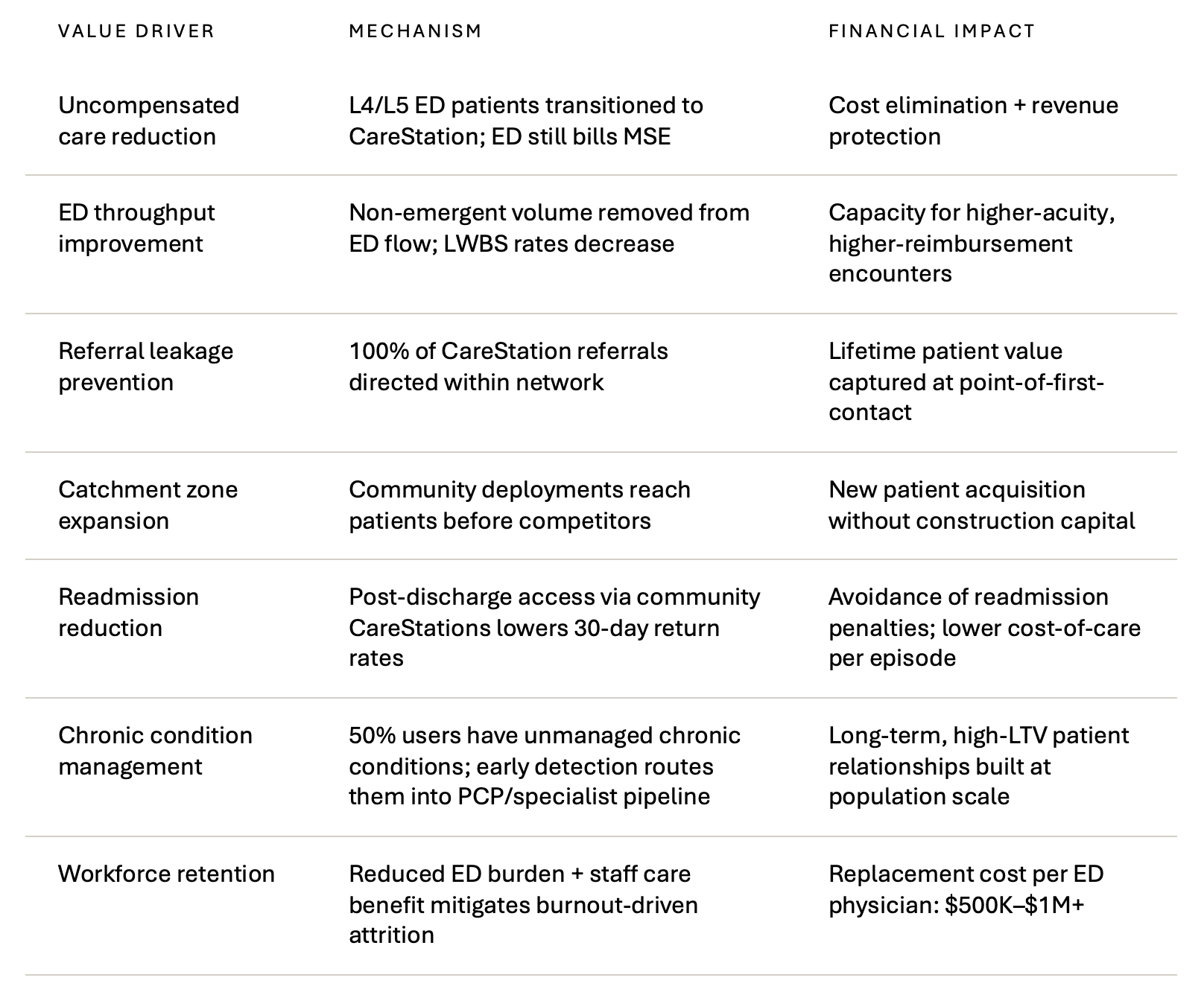
Every line in this table maps to a known, quantified problem your health system is already absorbing. Each CareStation deployment is an investment with identifiable, trackable returns.
The question is no longer whether your health system can afford to deploy CareStations. It's whether you can afford to be the last system in your market that hasn't.
Ready to See the Numbers for Your Healthcare System? Our health system strategy team will model the specific ROI opportunity for your patient population, ED volume, and catchment geography—at no cost and no obligation. Request a strategic assessment.
Sources & Citations
- [1]KFF Medicaid Enrollment and Unwinding Tracker. As of September 2024, over 25 million people were disenrolled during the unwinding of the COVID-19 continuous enrollment provision. kff.org, updated 2024.
- [2]KFF Medicaid Enrollment and Unwinding Tracker. Nearly 69% of those disenrolled lost coverage for procedural or paperwork reasons, not because they were ineligible. kff.org, 2024.
- [3]KFF / Pew Charitable Trusts analysis of Medicaid eligibility changes and projected enrollment impacts. Independent projections estimate 7.5 million newly uninsured by 2034 resulting from work requirements and documentation changes taking effect in 2027. kff.org / pew.org, 2025–2026.
- [4]McIntyre A et al., "Projected Health System and Economic Impacts of 2025 Medicaid Policy Proposals." PMC / JAMA Health Forum, 2025. Modeling projects ~94,800 preventable hospitalizations and 1.6M people delaying care annually by 2034.
- [5]Commonwealth Fund, "Reducing Medicaid Churn: Policies to Promote Stable Health Coverage." Loss of Medicaid coverage, even temporarily, leads to more hospitalizations and ER visits. commonwealthfund.org, June 2025.
- [6]Western Journal of Emergency Medicine (via Gumbo Health analysis). Average revenue loss per LWBS patient is approximately $687 in direct ED fees. getgumbo.com / WestJEM, 2024.
- [7]d2i Healthcare, "Reducing Left Without Being Seen, Against Medical Advice." Direct ED revenue loss of $500+ per LWBS; inpatient revenue losses of $10,000+ for patients who would have been admitted. d2ihc.com, 2021.
- [8]Sheraton et al., "Patients leaving without being seen from the emergency department." During a multicenter study period, 3.2% of 626,548 ED visits resulted in patients leaving before treatment was complete. JACEP Open / PMC, 2020.
- [9]Springer Internal and Emergency Medicine, "Characteristics and retention of emergency department patients who left without being seen." 78.1% of LWBS patients who returned to the ED did so within 72 hours; patients without follow-up tended to be younger, female, and non-White. link.springer.com, June 2021.
- [10]PubMed, "Nonurgent Emergency Department Visits by Insured and Uninsured Adults." Of all nonurgent ED visits, 77.9% were made by insured adults; insured nonurgent visits were more often made by female adults with a primary care provider. pubmed.ncbi.nlm.nih.gov, 2015.


.avif)












.avif)


.avif)




















































.avif)















